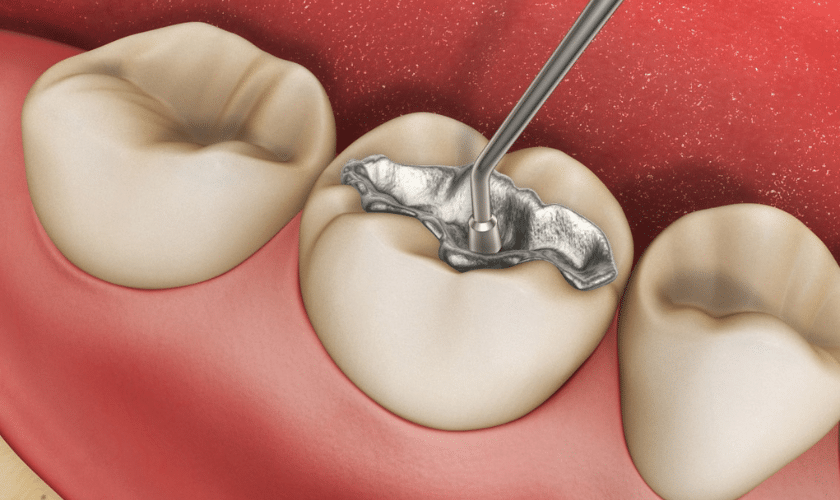
Histopathological mechanisms of tooth sensitivity after filling
Morphological Characteristics of Dentin
The structural composition of dentin is the primary variable in the development of post-restorative hypersensitivity. Dentin is permeated by microscopic channels known as dentinal tubules, which radiate from the pulp chamber outward to the enamel-dentin junction (DEJ).
Tubular Density and Diameter
The density of these tubules varies significantly depending on depth. Near the enamel, the tubular density is lower, and the diameter is smaller. However, as one approaches the pulp—in cases of deep caries excavation—the density increases to approximately 45,000 tubules per square millimeter, and the diameter widens. This morphological reality explains why deeper preparations are inherently more susceptible to tooth sensitivity after filling. The surface area of exposed fluid (liquor dentis) is exponentially higher in deep preparations, creating a direct pathway for hydrodynamic stimuli to reach the pulp tissue.
The Hydrodynamic Mechanism of Transduction
The prevailing scientific model for dentin sensitivity, established by Brännström, is the Hydrodynamic Theory. This model posits that the pain response is not a result of direct nerve stimulation, but rather a mechanical transduction process mediated by fluid dynamics.
Fluid Displacement Dynamics
The dentinal tubules are filled with a plasma-like fluid. When an external stimulus is applied to the restored tooth, it induces rapid fluid movement. Thermal stimuli are particularly potent drivers of this mechanism. Cold causes a contraction of the fluid volume, leading to outward flow, while heat causes expansion and inward flow. This rapid displacement generates a shear force within the tubule. The A-delta nerve fibers, which are myelinated and responsible for sharp, localized pain, are interwoven with the odontoblast processes. The hydraulic force distorts the odontoblast membrane, triggering the mechanoreceptors on the nerve endings. This sequence is the fundamental mechanism behind tooth sensitivity after filling.
Cellular Response: The Inflammatory Cascade
Beyond fluid dynamics, the restorative procedure induces a cellular inflammatory response known as reversible pulpitis. The friction and vibration of rotary instrumentation, even under adequate water irrigation, generate thermal energy that can damage the odontoblastic layer.
Vasodilation and Intrapulpal Pressure
In response to this cellular injury, the pulp tissue releases inflammatory mediators such as bradykinin and prostaglandins. These mediators cause vasodilation (widening of blood vessels) and increased capillary permeability. In soft tissues like skin, this would result in swelling. However, the dental pulp is encased in a low-compliance environment—rigid dentin walls. Consequently, the increased blood volume leads to a sharp rise in intrapulpal pressure. This pressure lowers the firing threshold of the nerve fibers, creating a state of hyperalgesia where even innocuous stimuli are perceived as painful. This inflammatory pressure is a key contributor to prolonged tooth sensitivity after filling.
Reparative Dentinogenesis: The Biological Cure
The biological resolution of sensitivity is dependent on the bio-activity of the pulp, specifically the process of tertiary dentin formation.
Reactionary vs. Reparative Dentin
If the original odontoblasts survive the trauma of the cavity preparation, they secrete reactionary dentin—a new layer of mineralized matrix along the pulpal wall. If the primary odontoblasts undergo necrosis due to the trauma, stem cells within the pulp differentiate into odontoblast-like cells to form reparative dentin. This new layer of calcified tissue acts as a biological barrier, effectively sealing the internal opening of the dentinal tubules. As this layer thickens over weeks or months, the permeability of the dentin decreases, the fluid movement is restricted, and the neural response subsides. This histological timeline correlates with the clinical reduction of post-restorative sensitivity.
The phenomenon of sensitivity following restorative procedures is a physiological intersection of fluid mechanics and inflammation. It represents the tooth's sensory detection of mechanical and thermal stress. Understanding the microscopic architecture of the dentin tubules and the hydrodynamic forces at play provides the scientific rationale for why tooth sensitivity after filling occurs and why biological healing requires a specific duration for the deposition of reparative dentin.